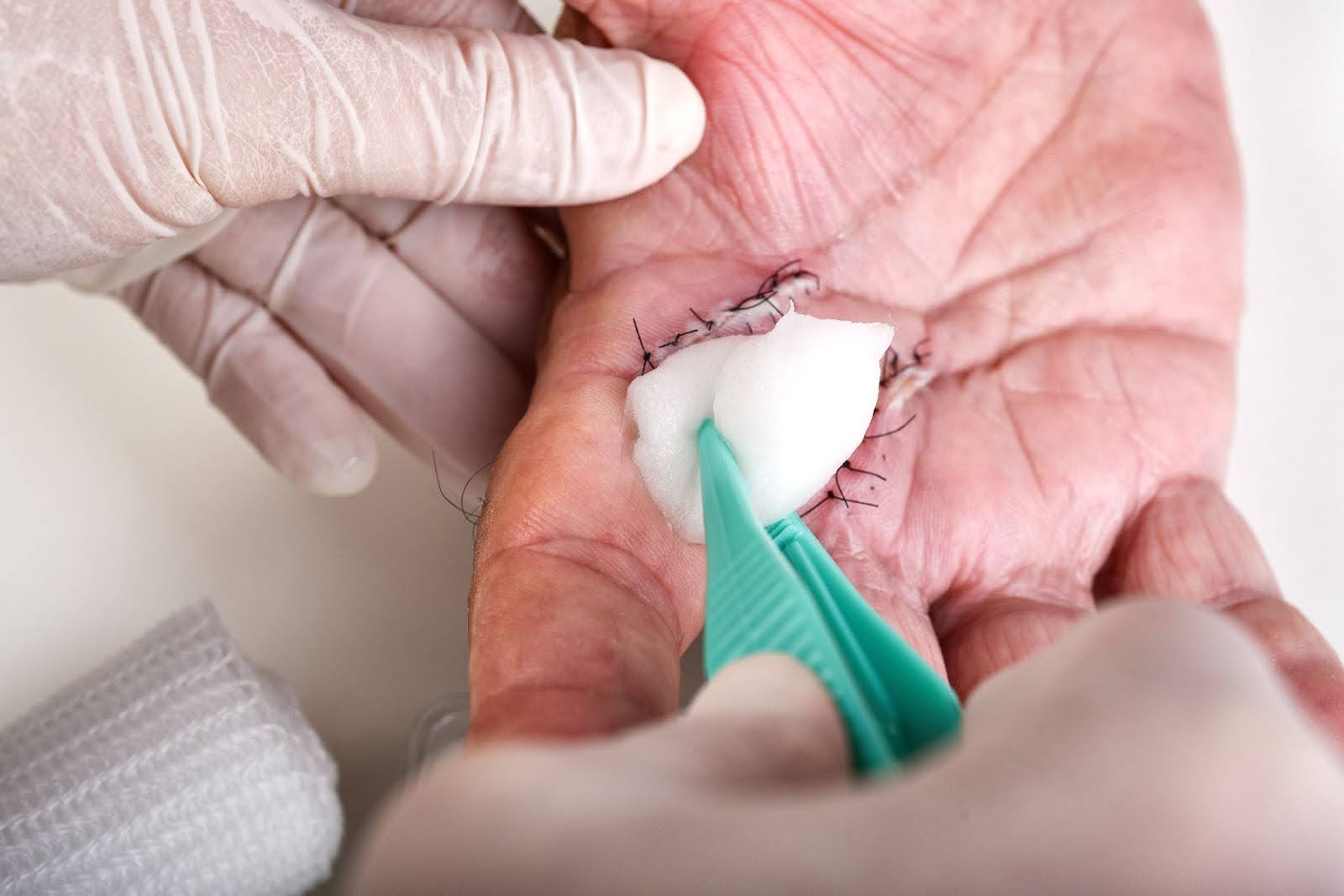
What is Wound Dehiscence and Why Does it Happen?
A healing wound should close securely, but sometimes it opens up instead. This condition, known as wound dehiscence, can cause setbacks in recovery and increase health risks. It often catches patients off guard, especially during the early stages of healing. Knowing why it happens and how to respond can make a difference between a smooth recovery and prolonged complications.
What is Wound Dehiscence?
Wound dehiscence occurs when a surgical or traumatic wound reopens after it has been stitched or closed. This separation may affect the top layer of skin or extend deeper into muscle or connective tissue. The risk of infection increases, and healing takes longer than expected. It may occur days or weeks after surgery, often during routine movement or when pressure is applied. Patients recovering from abdominal, chest, or orthopedic surgeries are more vulnerable. Awareness of this condition is vital for safe and successful healing.
Partial vs. Full-Thickness Wound Dehiscence
Partial dehiscence involves only the superficial skin layers, while full-thickness cases expose underlying tissue. The deeper the separation, the more complex the care required. Minor openings may be managed with proper wound care and dressing changes. Full openings often necessitate surgical revision and require monitoring for potential infection. Recognizing the level of separation early helps guide the correct response. Even a partial wound needs close attention to prevent it from worsening.
Emotional and Physical Impact on Recovery
Wound dehiscence can delay healing and impact mental well-being. Patients often experience fear, anxiety, or frustration during treatment setbacks. Physically, pain intensifies, and daily activity becomes more restricted. Medical expenses may rise due to repeat procedures or extended recovery periods. The emotional burden grows when healing progress suddenly reverses. A proactive response can reduce both stress and complications.
Why Wound Dehiscence Happens After Surgery
A combination of pressure, infection, and internal health conditions often triggers wound dehiscence. Each factor disrupts the normal post-surgical healing process in different ways. Understanding these causes helps surgeons, care teams, and patients take preventive steps. Identifying these issues early can support better outcomes for future surgeries and wound care plans.
Pressure and Physical Strain on Healing Tissue
Excessive tension or movement on the incision area can cause tissue to pull apart. It commonly occurs during coughing, lifting, straining, or when there is poor mobility support. Even a sudden movement, such as sneezing, can impact surgical sites. The tissue is more stressed in high-tension areas, such as the abdomen or joints. If sutures were too tight or improperly spaced, strain increases the chance of rupture. Surgeons must evaluate risk during the closure, and patients must protect their wounds afterward.
Infection Disrupts Tissue Formation and Stability
Infections weaken the body’s healing mechanisms by attacking tissue and introducing harmful bacteria. Surgical sites with poor hygiene, moisture buildup, or poor airflow become vulnerable. Infected tissue may not regenerate properly, leading to softening, drainage, or tissue breakdown. Antibiotics help, but it becomes harder to close once the wound is compromised. Clinicians must detect early signs such as redness, swelling, and odor to intervene quickly. Strong immune function and sterile conditions are key to healing.
Health Conditions That Increase Wound Risk
Diabetes, obesity, vascular disease, and poor nutritional status slow down tissue recovery. These conditions reduce oxygen supply, compromise immune function, or increase tension at the wound site. For example, high blood sugar levels impair the activity of white blood cells, thereby increasing the risk of infection. Obesity adds physical pressure and limits blood flow, while smokers have reduced circulation and collagen production. Medications like steroids also interfere with healing. Pre-surgery assessments should account for these risk factors to build personalized care plans.
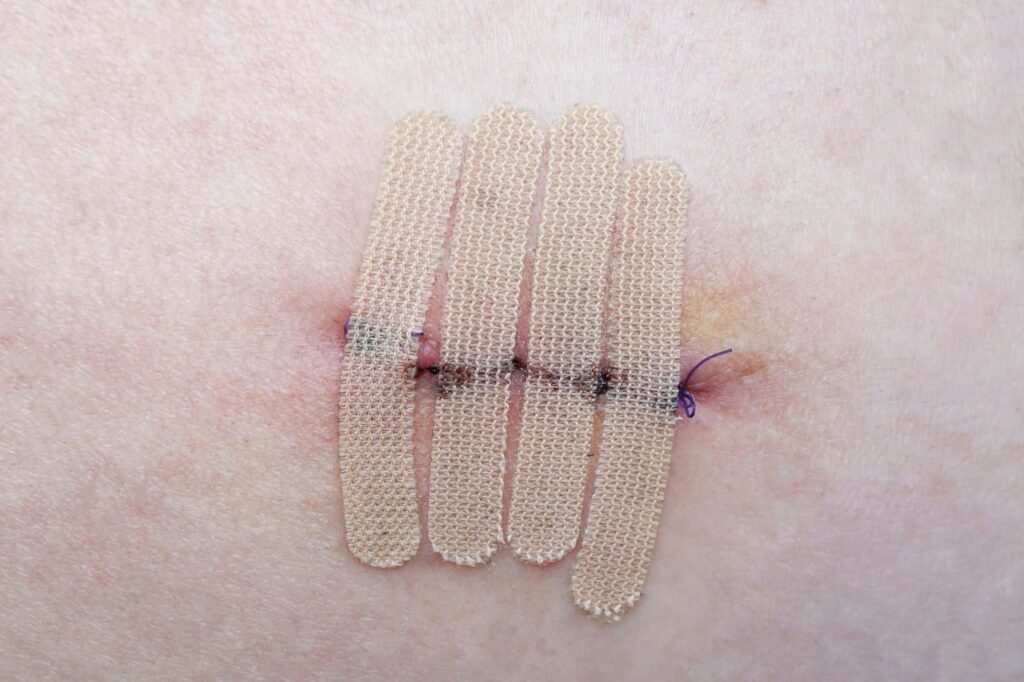
Environmental and Aftercare Factors That Interfere
Poor wound care after surgery plays a significant role in dehiscence. Ignoring hygiene, skipping dressing changes, or applying the wrong ointments can weaken skin closure. Wearing tight clothes, sleeping on incisions, or reusing old bandages invites contamination. Failure to follow up with healthcare providers may delay detecting early wound issues. A clean environment and proper rest improve healing speed and reduce risk. Patients must treat surgical sites as medically active areas, not just scars.
How to Recognize Wound Dehiscence Symptoms
Wound dehiscence often starts with subtle physical changes that escalate quickly. Patients should monitor the incision site and their entire body for signs of complications. Understanding these symptoms improves the chances of early detection and successful treatment. Caregivers and medical professionals should be trained to recognize these red flags immediately.
Visible and Sensory Clues at the Wound Site
One of the earliest signs is visible separation of the wound edges. The site may appear broader, deeper, or more inflamed than before. Patients often report a stinging or pulling sensation near the area. Drainage may increase, turning yellow, green, or bloody. A foul odor, increased warmth, or redness are classic signs of infection. These symptoms should never be dismissed as “normal healing.”
Systemic Warning Signs to Take Seriously
Dehiscence can sometimes trigger full-body symptoms, such as fever, chills, fatigue, or a rapid heart rate. These can suggest the spread of infection or internal inflammation. Blood pressure may drop in severe cases, or confusion may develop if sepsis begins. Patients recovering at home should track their daily feelings, not just the appearance of the wound. Even mild systemic symptoms, paired with wound changes, warrant a medical evaluation. Ignoring them can escalate the situation in hours.
When to Contact a Doctor or Visit Urgent Care
Contact your provider immediately if the wound looks deeper, smells bad, or leaks heavily. Any increase in pain, swelling, or redness should be reported, especially if paired with fever. Avoid applying ointments or tightening bandages without first consulting your healthcare provider. Healthcare providers may need to remove dead tissue, apply new dressings, or prescribe antibiotics to manage the condition. Delayed intervention may lead to hospital readmission or surgical repair. Timely medical input is always safer than self-diagnosing.
Treatment Options for Wound Dehiscence
Wound dehiscence treatment depends on the depth of the separation and underlying causes. While minor cases heal with wound care and observation, others require more complex intervention. Treatment aims to clean the wound, prevent infection, and help it close properly. Each step reduces risks and supports long-term healing.
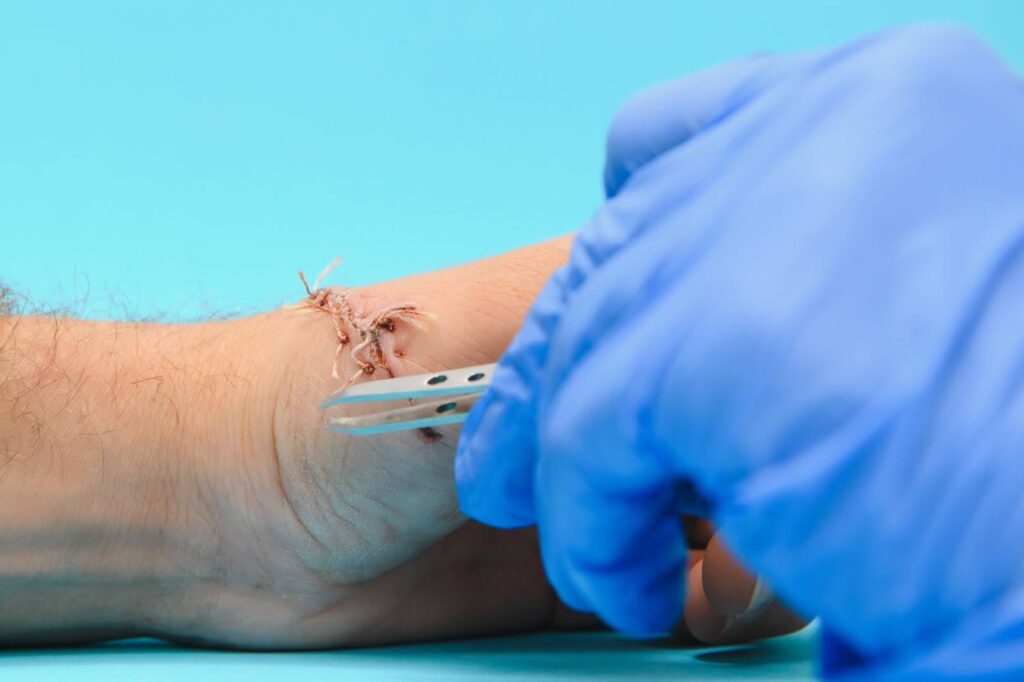
Wound Cleaning and Local Care Techniques
Medical professionals clean the wound with sterile solutions to remove debris and bacteria. Dressings are changed regularly to protect the site and monitor progress. In some cases, dead tissue is removed in a process called debridement. Depending on the infection level, antibiotic ointments or systemic medications may be used. Negative pressure wound therapy (vacuum-assisted closure) is often used for moderate cases. These steps create the best environment for tissue repair.
Surgical Repair for Deep or Worsening Wounds
When wounds are too deep or unstable, surgical re-closure becomes necessary. Surgeons may use sutures, skin flaps, or grafts to strengthen the wound. These procedures reduce tension and close gaps that cannot heal on their own. The new closure must be monitored to prevent another rupture. Recovery from re-suturing involves longer rest periods and tighter movement restrictions. Some cases also require hospital stays for intravenous antibiotics or drainage systems.
Follow-Up Care and Healing Monitoring
Treatment does not end once the wound is closed. Patients return for regular check-ups to confirm tissue strength and look for complications. Adjustments in medication, wound care products, or lifestyle may be needed. Blood tests may be taken to track inflammation or infection markers. Nutritional plans often include zinc, protein, and hydration goals. These elements contribute to healing acceleration by supporting cell growth and tissue repair. Full recovery depends on consistent follow-through and proper support.
Preventing Wound Dehiscence After Surgery
Wound dehiscence prevention begins before surgery and continues until the wound has fully healed. A mix of good surgical practices, patient education, and proper post-op care makes a measurable difference. Every decision along the recovery path helps prevent complications. Knowing how to support your wound is just as crucial as the procedure itself.
Steps Patients Should Take Before Surgery
Patients should prepare by optimizing their health status. That includes managing chronic conditions, quitting smoking, improving nutrition, and maintaining cleanliness. Surgeons may recommend pre-op vitamins or specific wound-prep protocols. Following fasting or bathing instructions is essential to avoid contamination. Avoiding unnecessary medications that affect blood flow or immune function is also part of the plan. The stronger the body before surgery, the smoother the healing process.
Post-Op Habits That Protect Wound Sites
After surgery, movement should be careful and controlled. Patients must avoid lifting, twisting, or straining the incision area. Daily hygiene, fresh dressings, and good air circulation prevent infections. A balanced diet, hydration, and rest help rebuild tissue. Reporting unusual symptoms early gives doctors time to intervene. Success depends on sticking to the care plan without shortcuts.
Surgical Techniques That Lower Risk
Surgeons use tension-free closure techniques and high-quality sutures to secure incisions. In high-risk patients, mesh or skin reinforcement may be added. Selecting the right incision type and avoiding overlapping previous scars helps minimize stress on the skin. Closure method decisions are based on wound location, size, and tissue condition. Careful surgical planning directly reduces wound dehiscence rates. Trusted healthcare providers consistently apply these best practices.
Stop Wound Dehiscence Before it Starts
Wound dehiscence can turn a straightforward recovery into a long, frustrating process, but it doesn’t have to. Every decision, from how you move to when you ask for help, shapes how your body heals. Paying attention isn’t being cautious; it’s being in control. Trust your instincts, follow expert care, and treat wound healing like the priority it is. Recovery isn’t about perfection, but about staying aware and responding when your body speaks up. The right wound care solutions can distinguish between setbacks and steady progress. Start with the ones that work.
